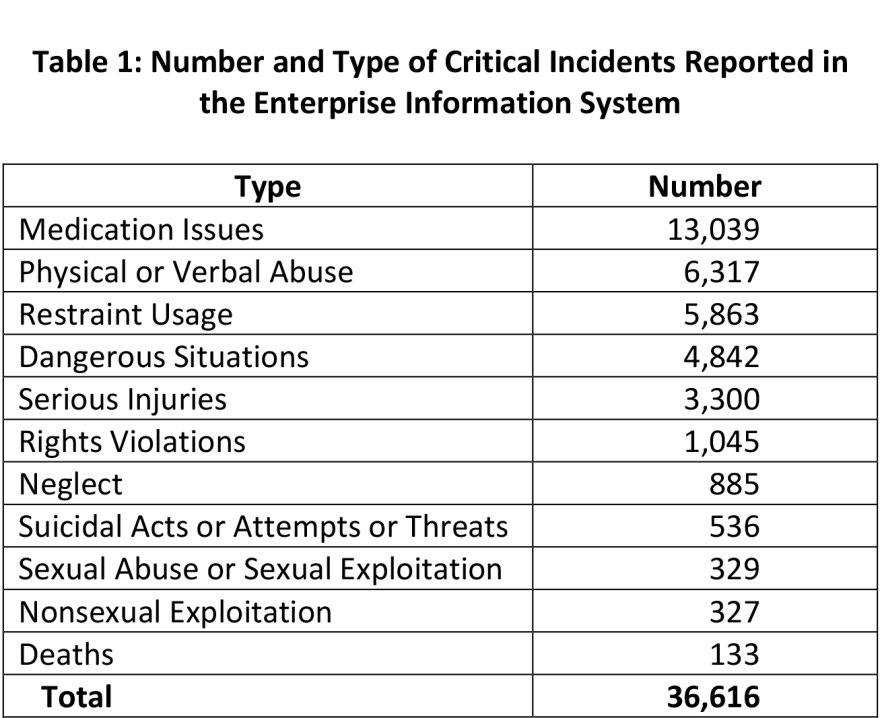
The state of Maine is failing to adequately protect people with developmental disabilities, according to a federal report released Thursday.
The U.S. Office of the Inspector General finds that both state and community-based providers do not properly report and investigate critical incidents involving the nearly 3,000 individuals in community based care.
During the recent two and a half year audit, 133 people with developmental disabilities in the Medicaid program died while under community-based care. Not one of those deaths was analyzed or investigated, including nine that the U.S. Health and Human Services Office of the Inspector General found were unexplained, suspicious or untimely.
One example, says Curtis Roy, an assistant regional inspector, involved a resident who drowned while taking a bath.
“That is just very, very troubling to me that this would happen and that somebody who should have been monitored more closely wasn’t. And as a result, appears to have drowned in a bathtub,” he says.
It’s just one example where Roy says Maine is failing to meet state and federal requirements to report critical incidents. That’s any event where the safety, welfare or rights of someone with a developmental disability has potentially been violated.
Deaths are one example. Emergency room visits are another. Roy says more than a third of those visits weren’t reported.
“We found that about 34 percent of the critical incidences involving these individuals were not reported by the community-based providers to the state agency,” he says.
The Inspector General’s report also found that DHHS did not investigate 95 percent of incidences of suspected abuse or neglect, and failed to immediately report such cases to a district attorney or law enforcement. Roy says DHHS also failed to make sure community based providers do internal reviews of critical incidents and did not conduct its own analysis to identify trends.
“In other words, they were not looking to see if certain providers had more critical incidences happening to their patients than others. Or if there was a certain type of critical incident happening at all of the homes,” he says.
“There’s a lack of reporting on the most egregious abuse. And there’s an over-reporting on stuff that does not necessarily rise to the level of abuse and neglect.” says Kim Moody, executive director of Disability Rights Maine.

The state is supposed to inform the organization about rights violations, but the Office of the Inspector General found that 20 percent were not reported. Moody says both DHHS and community-based providers share responsibility for the problem.
“These are people that didn’t go into this to abuse people. But there’s not enough accountability. There’s not enough money in the system,” she says.
Moody says the lack of sufficient reporting is a longstanding issue that’s not exclusive to the LePage administration. It’s also not exclusive to Maine.
The Office of the Inspector General has issued reports on Massachusetts and Connecticut, and found they too fail to properly report and investigate critical incidents. Though the reports focus on state agencies and community providers, Roy notes that hospitals in all of these states also failed to report as required by law.
“The mandated reporters based at the hospitals who have treated these people didn’t report a single incident of potential abuse or neglect to the state,” he says.
That’s of the incidents investigated. Jeff Austin of the Maine Hospital Association says he suspects the gap could be because patients or their caregivers may not communicate that there’s an issue to be concerned about.
“My assumption is that it’s just a difficulty in teasing that out, and not a lack of understanding or obligation to report,” he says.
The Inspector General’s report made seven recommendations to the state. Essentially, it wants DHHS to train its staff and community-based providers on proper protocol and to fully implement its own state regulations for critical incident reporting.
In a written response, the acting commissioner of DHHS, Ricker Hamilton, says the issues identified in the report happened during a time of transition and have since been addressed.
But the executive director of the Maine Association for Community Service Providers, Lydia Paquette, says she’s not aware of any improvements. In a written statement, Paquette says community service providers have repeatedly brought concerns to DHHS about critical incident reporting and made recommendations similar to those in the report.
This story was updated at 3:40 p.m. ET.